Full Mouth Rehabilitation Process Step by Step: A Specialist’s Clinical Guide
- Dr Samintharaj Kumar

- 11 hours ago
- 12 min read
What if the solution to a lifetime of dental frustration wasn't a series of quick fixes, but a single, meticulously engineered biological blueprint? In my clinical experience, many patients arrive at my practice feeling exhausted by years of difficulty chewing or the persistent embarrassment of a failing smile. I understand that the prospect of a total restoration can feel daunting, especially when you're faced with the complexity of a full mouth rehabilitation process step by step. It's not merely about aesthetics; it's about reclaiming your quality of life through a lens of clinical precision and patient-centred care.
As a clinician and founder, I believe that a successful outcome is rooted in transparency and logical progression. From a biological perspective, we must integrate advanced diagnostics and precise surgical protocols to ensure your new smile is as durable as it is natural. In this guide, I'll walk you through the multi-phase journey of total restoration. You'll gain a clear understanding of the timelines, the technology involved, and exactly what you can expect as we work together to restore both your function and your confidence.
Key Takeaways
Understand why total oral restoration is a biological necessity that reverses bone loss and muscular imbalance rather than just a cosmetic fix.
Learn how I utilise AI-assisted diagnostics to meticulously plan your full mouth rehabilitation process step by step for predictable, long-term success.
Discover the importance of clinical stabilisation and building a secure foundation through precision implantology and biological dentistry.
Explore the transformative impact of a restored bite on your facial aesthetics and the functional freedom to eat and speak without hesitation.
Table of Contents
Understanding the Need for Full Mouth Rehabilitation: Beyond Aesthetics
As a clinician and founder, I often meet patients who view their dental issues as a collection of isolated problems. They might have a few missing molars or some worn-down front teeth, but they don't yet see the interconnectedness of their oral health. A full mouth reconstruction is far more than a series of cosmetic enhancements; it's the comprehensive restoration of every tooth in both the upper and lower jaws. The goal is to return the entire masticatory system to a state of biological and functional harmony.
The science of oral decline is quite unforgiving. When teeth are lost or severely compromised, the underlying alveolar bone loses the mechanical stimulation it requires to remain dense. This leads to bone resorption. Over time, this loss of structural support causes the jaw to shift, creating a muscular imbalance that affects how you speak, chew, and even breathe. Understanding the full mouth rehabilitation process step by step begins with recognising that we aren't just fixing teeth; we're salvaging the structural integrity of your face.
To better understand this concept, watch this helpful video:
The Silent Progression of Oral Decline
One of the most profound consequences of tooth loss is the reduction of the vertical dimension of occlusion. This is the height between your nose and chin when your teeth meet. As this height collapses, it leads to "facial collapse," where the lips appear thinner and the chin protrudes, resulting in a prematurely aged look. This shift often triggers chronic TMJ disorders and headaches. It's a domino effect. The remaining healthy teeth take on excessive force, leading to fractures and further tooth loss. In my clinical experience, early intervention is paramount. Rebuilding the bite early prevents the need for more complex, invasive bone grafting procedures later on.
Why a Holistic Biological Approach Matters
From a biological perspective, my philosophy moves beyond the traditional "drill and fill" approach. I believe we must address the root causes of dental failure, such as systemic inflammation or gut health imbalances, to ensure long-term success. The mouth is the gateway to the body. Chronic oral infections can drive systemic issues, affecting everything from cardiovascular health to your immune response. As a specialist, I prioritise establishing a foundation of absolute health. We must eliminate infection and stabilise the oral environment before we ever consider placing permanent ceramic implants or restorations. The best outcomes begin with understanding the root cause.
The Step-by-Step Blueprint: Precision Diagnostics and AI-Assisted Planning
I often tell my patients that the best outcomes begin with understanding the root cause. When we embark on a full mouth rehabilitation process step by step, we aren't simply placing crowns; we're executing a meticulously engineered architectural plan. In my clinical experience, the failure of complex dental work often stems from a rushed diagnostic phase. By using AI-assisted diagnostics, I can detect hidden pathologies and evaluate bone density with a level of precision that was previously impossible. This allows us to map out a biological foundation that supports long-term stability.
Modern technology has transformed how I approach these cases. We utilise Cone Beam Computed Tomography (CBCT) and 3D intraoral mapping to create a "digital twin" of your mouth. This data is then fed into Digital Smile Design (DSD) software. This technology allows you to preview your final result before a single tooth is touched. It bridges the gap between clinical necessity and your personal aesthetic goals, ensuring there are no surprises during the final delivery.
Phase 1: Comprehensive Records and Digital Mapping
This initial stage involves rebuilding and/or replacing all of the teeth by first capturing thousands of data points. I map the intricate relationship between your teeth, jaw joints, and facial muscles. We don't just look at the teeth in isolation. We evaluate the TMJ (jaw joint) to ensure the new bite will be functionally stable. This collaborative process allows us to design your new smile aesthetics together, ensuring the final result complements your unique facial features. If you are curious about how these technologies can be applied to your specific case, a clinical consultation is often the most enlightening first step.
Phase 2: Deprogramming the Jaw and Bite Analysis
Before we can build, we must find your "true" bite. Many patients requiring full mouth care have developed compensatory habits due to missing or worn teeth. Their jaw muscles are often in a state of chronic tension. We use a deprogramming appliance to "reset" these muscles, allowing the jaw to settle into its most natural, relaxed position. From a biological perspective, this is critical. It allows me to analyse the vertical dimension of occlusion and plan how to restore a youthful facial structure. This clinical blueprint guides every subsequent surgical and restorative step, ensuring the final restorations feel as natural as they look. The right diagnosis changes everything.
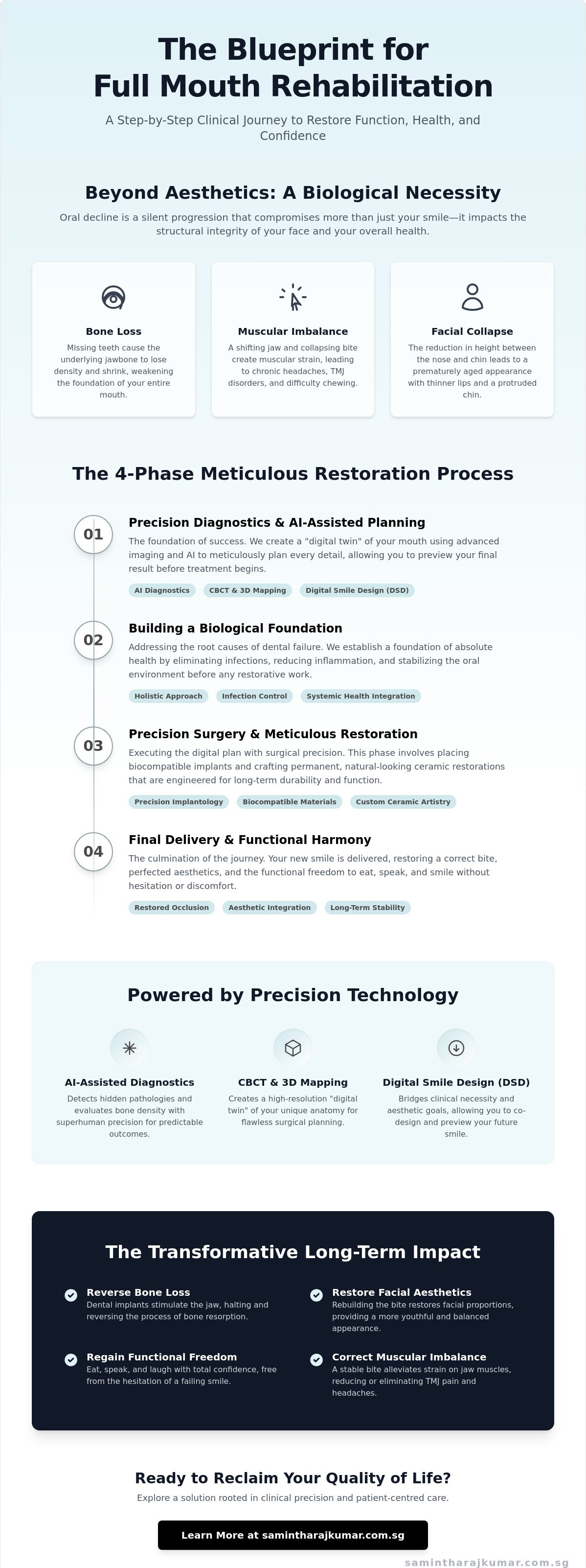
The Clinical Journey: Executing the Rehabilitation Process
Once the digital blueprint is finalised, we move from the visionary phase to clinical execution. As a clinician and founder, I view this transition as the moment our architectural planning meets biological reality. The full mouth rehabilitation process step by step requires a disciplined adherence to surgical and restorative protocols. We aren't just replacing teeth; we're performing a comprehensive dental treatment that restores the entire oral ecosystem. This journey involves several distinct phases, each designed to ensure the foundation is as resilient as the final result.
We begin with Phase 3, which focuses on biological stabilisation. This involves the meticulous removal of any active infection, failed previous restorations, or teeth that cannot be salvaged. I believe we must create a sterile, healthy environment before introducing any new materials. Following this, Phase 4 establishes the surgical foundation. This is where we place dental implants or perform bone grafting. For many, this is the most anticipated part of the full mouth rehabilitation process step by step, as it sets the structural stage for everything that follows.
Biological Stabilisation and Foundation Building
In my clinical experience, the success of a rehabilitation depends entirely on the health of the surrounding tissues. We address gum disease and decay with absolute precision. From a biological perspective, I often recommend ceramic dental implants for patients seeking a metal-free, highly biocompatible alternative. These implants integrate beautifully with the soft tissue, reducing the risk of inflammation. For patients with severe bone loss, I utilise advanced protocols such as Zygomatic or Pterygoid implants. These specialised techniques allow us to anchor restorations in the stable bone of the cheek or the back of the jaw, often bypassing the need for extensive, multi-year bone grafting procedures.
Phase 5 is the transitional phase. During this time, you wear high-quality temporary restorations. These aren't just placeholders. They serve as a "test drive" for your new bite, allowing us to evaluate phonetic clarity, chewing efficiency, and aesthetic balance. We monitor how your jaw muscles adapt to the restored vertical dimension before proceeding to the final stage.
The Art of the Final Restoration
The journey concludes with Phase 6: the final restoration. This is where we fit the definitive ceramic or porcelain bridges. I prioritise handcrafted ceramics because they possess the strength and natural light-reflecting properties of real enamel. We don't settle for "good enough." We perform minute adjustments to the occlusion, ensuring the forces of your bite are distributed perfectly across the new restorations. This precision is what guarantees the longevity of the rehabilitation. A durable, natural-looking smile is the result of never compromising on the details. The best outcomes begin with understanding the root cause.
My Perspective: The Philosophy of Meticulous Restoration
I view every full mouth case as an architectural challenge. It's not just about placing individual restorations; it's about engineering a system where biology and mechanics exist in perfect equilibrium. As a clinician and founder, I've seen how a fragmented approach to dental care often leads to failure. When we follow a full mouth rehabilitation process step by step, we're ensuring that the final structure is as stable as it is beautiful. My philosophy is rooted in the belief that we shouldn't just fix what is broken. We must restore what was lost with a deep respect for the body's natural systems.
This perspective is what drives my commitment to innovation. Whether I'm designing a complex surgical guide or selecting a specific ceramic material, I'm thinking about how that choice will impact the patient ten or twenty years from now. I advocate for a visionary approach to dentistry that prioritises longevity and systemic health over short-term convenience. Every decision is deliberate. Every step is measured.
Why I Prioritise Ceramic and Biological Foundations
From a biological perspective, the materials we place in the mouth matter immensely. I advocate for metal-free, ceramic foundations because they are exceptionally biocompatible. In my clinical experience, metal-based restorations can sometimes lead to chronic gingival inflammation or greyish discolouration at the gum line. By choosing ceramic, we significantly reduce the risk of peri-implantitis, a leading cause of implant failure. My commitment to international protocols means I never compromise on material quality. We follow global standards of care to ensure that your new foundation supports long-term tissue health and systemic well-being.
Navigating Complex Cases: Zygomatic and All-on-4
I find particular purpose in helping patients who have been told they are not candidates for traditional implants due to severe bone loss. For these individuals, advanced protocols like All-on-4 dental implants or Zygomatic implants provide a path forward. These are not "off-the-shelf" solutions. They require the meticulous planning I discussed in earlier sections, often involving AI-assisted diagnostics to identify the most stable bone structures.
By utilising computer-guided surgery, we can achieve results that are both predictable and life-changing. I've watched patients transition from a state of constant pain and embarrassment to one of profound confidence. This isn't just about teeth. It's about the transformative power of a restored smile on a person's self-worth. If you are ready to explore how these advanced surgical techniques can rebuild your confidence, I invite you to learn more about my approach at samintharajkumar.com.sg. The best outcomes begin with understanding the root cause.
The Long-Term Impact: Life After Total Oral Rehabilitation
Completing the full mouth rehabilitation process step by step is more than a clinical milestone. It's a profound restoration of the self. In my clinical experience, the most rewarding moment isn't when the final bridge is cemented. It's when a patient returns for their first review and describes the simple joy of eating a meal without hesitation or pain. This functional renewal is the true measure of our success. By restoring the vertical dimension of your bite, we also achieve a natural aesthetic transformation. A properly supported jaw can take years off your appearance, smoothing the facial profile and restoring the youthful fullness of the lips.
The psychological shift is equally significant. I've watched patients reclaim their professional presence and social confidence after years of hiding their smiles. When you no longer fear the failure of a procedure or the discomfort of a mobile tooth, your focus shifts back to living your life. The right diagnosis changes everything. Seeing that transformation in my patients is why I'm so passionate about this field. From a biological perspective, we aren't just placing crowns; we're returning the body to a state of health that radiates through every social interaction.
Sustaining Excellence: Post-Rehabilitative Care
Maintaining these results requires a commitment to excellence that extends beyond the surgery. Regular specialist reviews are essential to monitor the integration of your ceramic implants and the health of the surrounding tissues. We also address lifestyle factors, such as managing bruxism through custom-fitted night guards, to protect your investment from excessive wear. Choosing a dental clinic with a long-term care philosophy ensures you have a partner in your health for the decades ahead. As a clinician and founder, I ensure my team prioritises this continuity of care to protect the legacy of your treatment.
The Future of Your Smile
Modern technology, from AI-assisted diagnostics to advanced biocompatible materials, ensures that a well-executed rehabilitation can last a lifetime. I view this work as a legacy of health and an investment in your future well-being. We've moved beyond temporary fixes to create a durable, biological foundation that stands the test of time. A restored smile isn't just a dental achievement. It's a testament to the transformative power of modern medicine and a commitment to your long-term quality of life. The best outcomes begin with understanding the root cause.
Reclaiming Your Quality of Life through Precision Restoration
Embarking on a full mouth rehabilitation process step by step is a profound commitment to your future health and self-worth. We've explored how AI-assisted diagnostics and a biological approach to ceramic implantology create a foundation that's as stable as it is natural. In my clinical experience, the most successful outcomes are achieved when we prioritise tissue health and functional harmony over quick fixes. A meticulous clinical blueprint ensures that every surgical and restorative stage is executed with absolute predictability.
As the founder of Nuffield Dental Holdings and a specialist in Zygomatic and All-on-4 protocols, I've dedicated my career to mastering these complex restorations. From a biological perspective, every detail we've discussed serves to ensure your new smile lasts for decades. The right diagnosis changes everything. Begin your journey toward total oral rehabilitation with a clinical consultation.
You don't have to live with the frustration of failing dental work or the embarrassment of a compromised smile. The path to total oral restoration is clear. With the right expertise and a patient-centred philosophy, your transformation is entirely within reach. I look forward to helping you reclaim the confidence you deserve.
Frequently Asked Questions
Is full mouth rehabilitation a painful process?
Modern clinical protocols and advanced sedation techniques ensure that the entire journey is remarkably comfortable. In my clinical experience, most patients report far less discomfort than they initially feared, often managing their recovery with standard over the counter medication. We prioritise a gentle, patient centred approach to ensure you feel secure and pain free throughout every surgical phase.
How long does the entire step-by-step process take?
The timeline for a full mouth rehabilitation process step by step typically spans several months, as it depends on your individual biological healing rate. While initial stabilisation and "Teeth in a Day" protocols can provide immediate functional results, the final integration of permanent ceramic restorations occurs once the bone and soft tissues have fully matured. This measured pace is essential for ensuring the long term stability of your new smile.
Can I get full mouth rehabilitation if I have severe bone loss?
Yes, severe bone loss is no longer a barrier to total oral restoration. As a specialist in Zygomatic and Pterygoid implants, I can anchor restorations in stable bone structures that bypass the need for traditional grafting. From a biological perspective, these advanced protocols provide hope for patients who were previously told they were not candidates for dental implants.
What is the difference between full mouth rehabilitation and a smile makeover?
A smile makeover primarily addresses the aesthetic appearance of the front teeth, whereas full mouth rehabilitation is a comprehensive functional and biological reconstruction. While a makeover might involve veneers for a brighter look, a rehabilitation restores the entire bite, corrects jaw alignment, and replaces missing teeth across both jaws. It is an architectural solution for complex oral decline rather than a purely cosmetic enhancement.
How much does the full mouth rehabilitation process cost in Singapore?
The investment for this procedure varies significantly based on the complexity of your case and the specific surgical protocols required. Factors such as the need for bone grafting, the type of implants chosen, and the number of restorations all influence the total investment. During a clinical consultation, I provide a detailed, transparent breakdown of the necessary steps to achieve a predictable and durable outcome.
What happens if I don't treat my failing teeth now?
Inaction often leads to a domino effect of systemic and structural decline. Beyond the difficulty of chewing, untreated tooth loss results in progressive bone resorption and the collapse of your facial height. This can trigger chronic TMJ pain, nutritional deficiencies, and a prematurely aged appearance. Early intervention is always the most conservative path to preserving your remaining biological health.
Will the final results look like natural teeth?
The final restorations are designed to be indistinguishable from healthy, natural teeth. We utilise handcrafted ceramics that mimic the light reflecting properties and translucency of natural enamel. By integrating Digital Smile Design, I ensure the size, shape, and shade of your new teeth perfectly complement your facial features and skin tone for a truly authentic result.
How do I maintain my new smile after the process is complete?
Maintaining your rehabilitation involves a combination of meticulous home care and regular specialist reviews. I recommend professional cleanings every six months to monitor the health of your implants and the integrity of the ceramics. For patients who grind their teeth, wearing a custom night guard is a vital lifestyle adjustment to protect your investment from excessive mechanical force.




Comments